This information is for people who have atrial fibrillation or who would like more information about it.
Atrial fibrillation is when the heart beats too fast in an irregular rhythm. It is caused by faulty electrical signals in your heart and is the most common type of arrhythmia (irregular heartbeat).
The different types of arrthythmia About atrial fibrillation What happens in atrial fibrillation? Symptoms of atrial fibrillation Complications of atrial fibrillation Causes of atrial fibrillation Diagnosis of atrial fibrillation Treatment of atrial fibrillation
About atrial fibrillation
Your heart is a muscular pump, responsible for delivering blood to the rest of your body. When your heart doesn’t beat in a normal way, it can’t do this as efficiently. Atrial fibrillation affects around 800,000 people a year in the UK. The condition mostly occurs in older people, affecting about seven in 100 people over the age of 65, although it can happen in younger people as well.
What happens in atrial fibrillation?
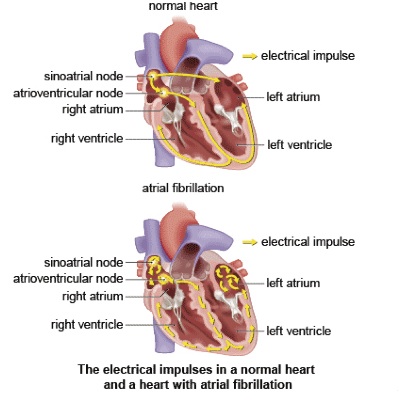
Your heartbeat is controlled by electrical signals (impulses), which travel through the heart making it contract. The signals travel from the atria (the upper chambers of the heart) to the ventricles (the lower chambers) through an area called the atrioventricular (AV) node. The AV node helps to synchronise the pumping action of the atria and ventricles.
Atrial fibrillation occurs when the electrical signals in the atria become disorganised, overriding the heart’s normal rate and rhythm. This causes the atria to contract irregularly or ‘fibrillate’.
There are three main types of atrial fibrillation:
paroxysmal – it happens over seconds, minutes or up to 48 hours and the heart returns to a normal rhythm by itself or with treatment
persistent – it requires electrical cardioversion to correct the rhythm permanent – even electrical cardioversion fails to restore the rhythm
Symptoms of atrial fibrillation
Symptoms of atrial fibrillation may include:
palpitations – you’re aware of your heart beating faster or in an irregular way chest pain or discomfort shortness of breath dizziness and light-headedness
Many people with atrial fibrillation only have mild symptoms, or don’t have any symptoms at all. These symptoms may be caused by problems other than atrial fibrillation. If you have them, visit your GP.
Complications of atrial fibrillation
Atrial fibrillation can cause a stroke and/or heart attack. This is because your blood isn’t flowing properly through your heart, so a blood clot can form. If a clot forms, it can block blood supply in your heart and cause a heart attack, or travel to your brain andcause a stroke. Because of this, people with atrial fibrillation are five times more likely to have a stroke than people without the condition.
If you have atrial fibrillation, you may need anticoagulant medicine (such as aspirin or warfarin) to prevent a clot forming.
Causes of atrial fibrillation
Many conditions that affect the heart or blood circulation can cause atrial fibrillation, including:
high blood pressure heart valve disease heart muscle disease (cardiomyopathy) coronary heart disease congenital heart disease (problems of the heart since birth) inflammation of the heart (pericarditis) thyroid diseases lung cancer and chest infections a blood clot on the lung (pulmonary embolism)
Certain factors can also trigger temporary, reversible atrial fibrillation, including:
alcohol being overweight caffeine certain medicines or drugs emotional or physical stress surgical procedures
Many people develop atrial fibrillation without having any underlying cause or risk factor. This is called lone atrial fibrillation.
Diagnosis of atrial fibrillation
Some people are not aware that they have fibrillation. If you have any concerns about your heart rhythm, see your GP. Your GP will ask about your symptoms and examine you. He or she may also ask you about your medical history.
Your GP will check your blood pressure, listen to your heartbeat and take your pulse. If your pulse is irregular, you are likely to have a test called an electrocardiogram (ECG). An ECG measures the electrical activity in your heart to see what the heart rhythm is.
If your GP suspects you have atrial fibrillation, he or she may refer you to a cardiologist – a doctor who specialises in identifying and treating heart and blood vessel conditions. You may have other tests in hospital, including:
blood tests
echocardiogram – an ultrasound scan of your heart providing a clear image of your heart muscles and valves that shows how well the heart is working
ambulatory ECG – this takes a recording of your heartbeat while you go
Treatment of atrial fibrillation
There are many treatment options available for atrial fibrillation. Your treatment will be tailored to you, and will depend on your own symptoms and the cause of your atrial fibrillation. Your doctor will discuss your treatment options with you.
The aim of treatment is to control your heart rhythm and rate, and reduce your risk of stroke or heart failure. You may not need any treatment at all, especially if your symptoms are mild.
Self help
Your doctor may suggest you improve your heart health by:
doing moderate exercise for 150 minutes (two and a half hours) over a week in bouts of 10 minutes or more, for example by carrying out 30 minutes on at least five days each week
eating a balanced diet with five portions of fruit and vegetables every day stopping smoking reducing alcohol and caffeine intake
Medicines
There are several different types of medicine that can help control atrial fibrillation, including beta-blockers, calcium channel blockers, anti-arrhythmic medicines and digoxin. They all work in different ways to control your heart rate or restore a normal rhythm.
Your doctor may prescribe a combination of any of these medicines. You may have to take them for just a short period until you have other treatment such as electrical cardioversion to restore your heart rhythm, or you may have to take them for months or years. Alternatively, you may be given medicine to take just when you get symptoms. If your atrial fibrillation has come on suddenly, you may be given anti-arrhythmic medicine, as tablets or through a vein to try and get your heart rhythm back to normal (this is called chemical or medical cardioversion), and is usually given within 48 hours of having symptoms.
Medicines to reduce your risk of blood clotting are called anticoagulants. These include warfarin, heparin and aspirin. You will probably be offered one of these in addition to any other treatments you have.
Always ask your doctor for advice and read the patient information leaflet that comes with your medicine.
Electrical cardioversion
An electric shock is used restore your heart’s normal rhythm. It’s usually given if your symptoms have lasted longer than 48 hours and chemical cardioversion has failed. Electrical cardioversion is less likely to work if the arrhythmia has been present for over a year. It’s also not suitable if the irregular rhythm is coming and going, since it’s most likely that arrhythmia will return after treatment. For more information see Related topics.
Surgery
Surgery is only used when your atrial fibrillation hasn’t responded very well to other treatments, and may include the following:
Pacemaker – a small device is implanted under the skin near your collarbone. It monitors your heartbeat and produces electrical signals to prevent pauses in the heart rhythm.
Catheter ablation – small tubes called electrode catheters are passed into your veins in the groin and threaded up to the heart. Abnormal tissue or the AV node, the junction box between upper and lower chambers (this is called AV node ablation) which is disrupting the electrical signals in your heart is burnt or frozen. You will also need a permanent pacemaker.
Anaesthesia is general and this will be discussed with your anaesthetist before your procedure is carried out.