International Federation for the Surgery of Obesity (IFSO); https://www.ifso.com 1997
The formula for calculating BMI = weight (kg) / (height) 2 (m2)
Grade I light (BMI = 30 kg/m2 34.9)
Grade II moderate (BMI = 35 kg/m2 39.9)
Grade III or severe morbid obesity (BMI over 40 kg/m2)
superozhirenie morbid (BMI greater than 50 kg / m)
Today, obesity is considered as a problem of individuals who are overweight, and as a worldwide pandemic infectious nature, which causes many health problems (diabetes mellitus type II, hypertension, sleep apnea syndrome, atherosclerosis, increased risk of heart attack, stroke, cancer) and significantly reduces life expectancy.
In the U.S., it is from the immediate complications of obesity die each year 260-380 thousand people. This surpasses the total mortality from lung cancer (154 OOO), colon (48 OOO), breast (40 000) and prostate (30 200).
Obesity significantly reduces life expectancy with an average of 2-5 years, with a slight excess body weight and 15-20 years with a BMI over 45 kg / m. In fact, two-thirds of all deaths caused by diseases associated with disorders of fat metabolism or actually obese.
The results of numerous clinical and experimental studies have provided strong
proved by the fact that so far no effective conservative policies for the treatment of patients with morbid obesity (BMI> 40 kg/m2). In 95% of patients after conservative therapy lost weight reduced or increases (in excess of the initial BMI) in the time interval 6 months – 2 years after treatment.
It is generally recognized that now only surgical treatment – is the only real method of effective medical care to patients with morbid obesity.
Why do we offer the most complex of all the available methods of surgical treatment of obesity?
This technique was developed by US Prof Hess and Canadian Prof. Marceau more than 30 years ago. Building on the experience of their predecessors and their personal, in the performance of other simplified methods, and sometimes deliberately harmful and ineffective, they studied the physiological aspects of obesity and come to a new, albeit complex, the technical, pathogenetically substantiated method of this operation.
It was found that overweight people have a genetic predisposition inherited, often reach the small intestine, which absorbs all the nutrients – fats, proteins and carbohydrates, a lot more than the average person, and in contrast, leaves no 4,0 – 4 5 m, and sometimes up to 7.5 m
Passage of food masses, that is, the promotion of food through the digestive tract in people who are overweight, considerably slowed down, which allows the small intestine to absorb the maximum amount of these proteins, fats and carbohydrates.
By studying the hormonal activity of the stomach, the researchers found that the “bottom” of the stomach are hormone – producing cells, which produce the hormone – ghrelin. Increasing this hormone is active and sometimes unrestrained appetite, desire to constantly nourish your stomach, what-react pleasure hormones – endorphins. This hormonal relationship creates dependence in humans by type of alcohol or drugs. Many patients become food addicts.
All this prompted the authors to propose a new method of its patients with all the factors of the disease.
At the first stage of the operation is carried out “hose” gastrectomy “Sleeve gastrectomy”, which reduces its volume, eliminate hormonally active zone, maintaining the physiological integrity of the body.
Patient before the surgery Patient 5 months after surgery 9 months after surgery



What is the difference of the operation of the widely proposed bypass surgery of the stomach, when also created a “mini” stomach?
With this method part of the stomach is removed in a vertical direction, thus reducing the volume removed gormonprodutsiruyuschaya zone.
With gastric bypass surgery, the imposition of “ribbon” on it, or other similar transactions, the stomach is reduced by its intersection horizontally, which does not affect its “bottom”, and therefore does not deprive a patient after surgery appetite, but just does not give him the opportunity to satiate the stomach the same volume. Such patients are in need of high-calorie, sweet foods often that doctors affectionately referred to as “a symptom of a sweet tooth.” In fact, such a patient can be compared to a drug addict, facing a “break” in the forced absence of “fun.” He repeatedly offered to support a diet, denying themselves the pleasure is what he wants.
Patients who had a ‘vertical gastric resection, “deprived of that painful feeling. The desire to feed your body all the time – lost. Saturation in small portions is fun. Removing hormone area often gives a paradoxical effect when the patients after surgery mark change preferences from sweet to sour, with meat products plant. But this is not a big deal because patients do not become addicted to food, and can as an ordinary person to control their desires.
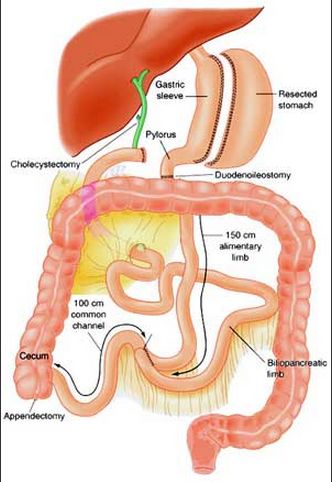
Quite a new and very efficient Hess-Marceau surgery – Bilio Pancreatic Bypass Surgery
Bypass Surgery
Patients with a low excess weight not exceeding a body mass index 40 kg/m2, this stage of the operation can be offered as a self-treatment, because it gets rid of the guaranteed 30 – 50 pounds overweight. However, if a patient with such a mass have diabetes mellitus type II, the application of this stage is not only free him from diabetes and such patients, as well as in patients with a body mass index greater than 40 kg/m2, you must complete the second phase of the operation – biliopankreatic bypass.
Gastric Band
A gastric band is a silicon band that’s placed around the stomach to diminish its capacity. A person will feel rapidly full, aiding the weight loss process. Gastric banding has many advantages such as: it is reversible; minor incisions are used; and it has a smaller complication rate than many other weight loss surgeries.
Gastric Sleeve
Is a relatively new procedure where approximately 60 % of the stomach is cut, thus considerably decreasing its capacity.
Intragastric Ballon
There is minimal risk in this procedure. No surgery is involved in this procedure. Under minimum sedation, through endoscopy a balloon is placed in the stomach, thus creating less room for food and a sense of being full more quickly.